Visiting the dentist can be particularly challenging for individuals with sensory sensitivities, as the typical dental environment is filled with potential triggers. However, with the right approach and preparation, these challenges can be mitigated, ensuring that dental care remains a priority without causing undue stress.
Sensory Challenges in Dental Care

The sensory-rich environment of a dental office poses unique challenges for individuals with heightened sensitivities, each element contributing to a potential overload that can make dental visits particularly daunting:
- Touch: The tactile experience in a dental setting is often intense. The sensation of dental tools operating within the mouth involves vibrations, poking, and scraping, which can provoke significant anxiety. Textures such as the rubbery feel of gloves or the hardness of dental instruments can also be unsettling. These sensations are sometimes unexpected and can trigger a strong anxiety response in those who are particularly sensitive to touch.
- Sound: Dental offices are notorious for their distinctive sounds, with the high-pitched noise of dental drills being one of the most universally recognized—and dreaded—aspects. Other equipment, such as suction devices and ultrasonic cleaners, also contribute to the cacophony, creating an auditory environment that can be extremely jarring. For individuals with auditory sensitivities, these sounds can amplify stress, making the dental experience much more challenging.
- Smell: The mix of odors in a dental office can be striking and unpleasant to many, particularly to those with heightened olfactory senses. Sterilizing chemicals, scented dental products, and the distinct smell of latex can combine to create a potent and often overpowering aroma. These smells can linger and permeate the space, making it difficult for someone with sensitive smell to relax and breathe comfortably during their appointment.
- Sight: Visual stimuli in a dental office can also contribute to sensory overload. Bright overhead lighting is necessary for dentists to perform precise operations but can be harsh and uncomfortable for patients, especially those with light sensitivity. Additionally, the close proximity of dental staff working near the face, along with the limited personal space while seated in the dental chair, can heighten feelings of vulnerability and discomfort.
- Taste: The flavors associated with dental procedures can be particularly distressing. Many dental products, such as mouthwashes, topical anesthetics, and fluoride treatments, have metallic or chemical tastes that can be unpleasant or even cause gagging. For individuals with taste sensitivities, these flavors can exacerbate the challenge of undergoing dental treatments, adding another layer of discomfort to the experience.
Strategies for Navigating Dental Visits
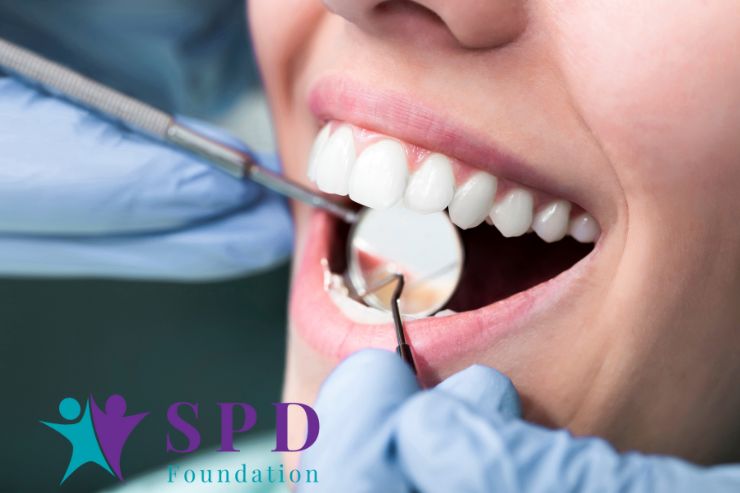
Effective planning and communication with your dental care provider can transform the experience:
- Choosing the Right Dentist: It’s essential to select a dentist who is experienced in dealing with sensory sensitivities. A preliminary discussion about their familiarity with sensory challenges will help ensure they are a good fit.
- Communicating Needs: Advance communication is key. Informing the dental team about specific triggers allows them to make necessary adjustments. For example, scheduling visits during quieter times can reduce auditory stress.
- Extended Appointments: Request longer appointment times to allow for breaks. This helps manage the sensory overload by providing periods of rest and recovery during the visit.
- Personal Comfort Tools: Bring items that help manage sensory input, such as noise-cancelling headphones to listen to calming music, which can mask the distressing sounds of dental tools.
- Pre-visit Orientation: Arrange a visit to familiarize yourself with the dental office and equipment. This can decrease anxiety by making the environment feel more predictable and less intimidating.
- Preventive Measures: Discuss with your dentist the possibility of using anti-anxiety medications or topical anesthetics to ease discomfort and anxiety before procedures.
Leveraging Resources and Community Support
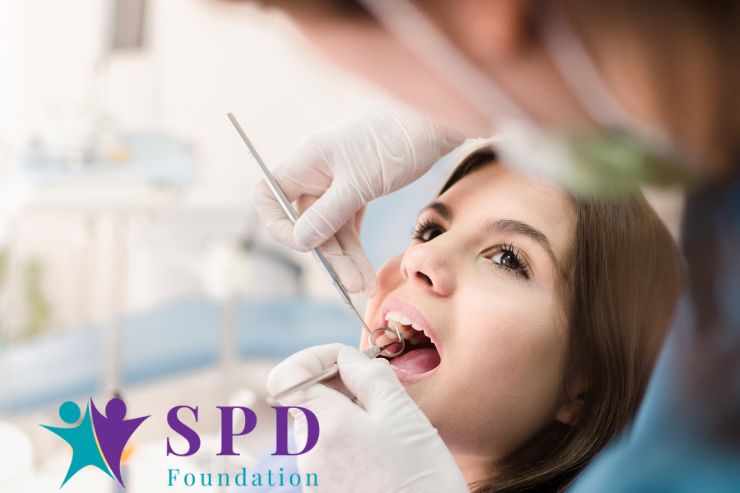
There is a wealth of resources and community support available to help navigate the complexities of dental care with sensory sensitivities:
- Organizations: Groups such as the Sensory Processing Disorder Foundation and the STAR Institute play a vital role in providing support for those with sensory sensitivities. These organizations offer a wealth of educational materials that help patients, families, and caregivers understand and manage sensory challenges more effectively. Additionally, they maintain comprehensive directories of healthcare providers who specialize in sensory issues. This can be an invaluable resource for finding dentists who are experienced in treating patients with heightened sensory awareness, ensuring a more tailored and sensitive approach to dental care.
- Helplines and Forums: Organizations like Autism Speaks and the Autism Society offer helplines and manage online communities that are essential for connecting with others facing similar challenges. These platforms allow individuals to exchange stories, advice, and support. Engaging with these communities can be incredibly reassuring and informative, offering new strategies for managing sensory sensitivities and fostering a sense of solidarity and understanding among its members. These forums also serve as a bridge to additional resources, such as expert advice or upcoming events that focus on sensory processing.
- Preparation Tools: These organizations frequently provide specific tools designed to prepare individuals for dental visits. These resources might include detailed checklists that help plan and execute a visit to the dentist with minimal stress, or tips on how to discuss sensory issues with dental professionals effectively. Preparation tools can also offer guidance on creating a sensory-friendly environment during dental appointments, such as using calming techniques or bringing personal items that help manage sensory input. These tools are designed to empower patients and caregivers to take proactive steps in managing dental care in a way that respects and accommodates sensory sensitivities.







